FOR most horse owners, colic is a nightmare situation and while it is undoubtedly a major cause of death in horses of all ages, it is also one of the most common conditions encountered and treated by veterinary surgeons.
There are a huge number of potential causes of colic but in about 90% of cases these can be easily resolved with treatment from your veterinary surgeon at home.
The tricky part is telling the difference between those cases which are relatively harmless from those which are life-threatening.
Is it colic?
“Colic” simply refers to signs of abdominal pain, these can include restlessness, pawing, looking at or kicking theflanks, sweating, lying down or rolling.
Some horses may simply seem a little depressed or off their feed while others can thrash around violently, potentially injuring themselves or those around them.
While the degree of pain is often an indication of severity, this is not always the case and it is not possible to make diagnosis based on symptoms alone.
Types of colic
Most cases of colic relate to an abnormality affecting the gastrointestinal tract causing pain due to spasm, stretch, irritation or loss of blood supply to part of the digestive system. Signs of colic can also occur in horses with bladder or reproductive issues, injuries, lameness, laminitis, ‘tying-up’, choke and even those with a fever.
There are countless causes of “true” gastrointestinal colic, which can range from mild cramps or spasmodic colic to life-threatening ‘twisted guts’ so the challenge is differentiating between these. Often, no specific diagnosis is reached and many horses with mild colic signs may recover uneventfully with treatment from your veterinarian.
Below are some of the more common categories of colic we encounter, but it is important to recognise that the potential causes of colic are wide, diverse and extend beyond those outlined below.
Spasmodic/gas colic: We probably see these most frequently and they commonly occur in horses after a change of diet or management such as being turned out onto fresh grass.
The horse experiences cramping due to spasm in the guts and gas accumulation. Usually the gut sounds will be louder and more active than normal but this type of colic usually responds wellto pain relief and anti-spasmodics.
Impaction colic: In these cases, a build up of feed or droppings occurs in part of the gut which becomes dry and firm and difficult to pass. Impactions occur most commonly in horses after a change of diet or management, especially horses which are on box rest due to injury or stabled on straw. An increase in dry fibrous feed combined with slower gut movements due to reduced exercise are usually to blame.
Horses may be dull, off feed or simply spend more time lying down in addition to more typical colic signs. A reduction in the number of droppings in the horse’s stable or the presence of dry droppings may be a clue that an impaction is present. Most cases are easily diagnosed on a rectal exam where the impaction can be palpated and respond to medical treatment with pain relief and fluids or oils given by stomach tube to soften the droppings.
Displacement colic: These occur where part of the bowel moves into the wrong location within the abdomen affecting the normal passage of gas and droppings.
Many cases can respond to medical treatment with pain relief and sometimes fluids and careful exercise, while other more persistent cases may require surgery to reposition the bowel.
Small intestinal strangulation: This is a more severe type of colic, commonly referred to as a twisted gut and can occur in a number of ways. The outcome is a complete blockage of the affected intestine as well as a loss of blood supply. Affected horses are usually in a lot of pain and can quickly become extremely sick, these cases require surgery to correct the twist and often remove the affected segment if it has become severely damaged.
Large colon torsion: In these cases, the large bowel rotates on itself creating a complete blockage and loss of blood supply. The symptoms are similar to small intestinal strangulation and life saving surgery is required to correct the twist.These colics are commonly seen in broodmares and are thought to occur due to the increase of space in the abdomen after foaling.
Signs of colic may also be seen in horses suffering from gastric ulcers and prior to or during a bout of diarrhoea.
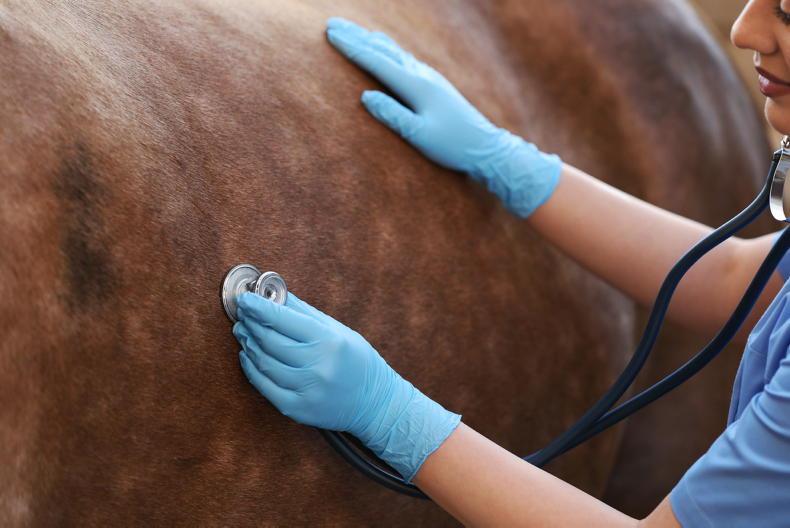
Your veterinary surgeon will usually start by examining your horse’s behaviour and degree of pain followed by a full physical examination including listening to the heart rate and breathing sounds, intestinal sounds, taking a temperature and checking the colour of the gums.
Response to pain relief is an important diagnostic tool and sedatives and painkillers are often administered after the initial assessment to see how the horse improves. For this reason, it is important not to give your horse any drugs before your veterinary surgeon arrives, unless you have checked with them first.
Further investigation will usually involve a rectal exam where your veterinary surgeon feels for signs of distension or displacement of parts of the gut, or the presence of an impaction (accumulation of feed material or droppings in part of the gut).
While this is a vital component of the evaluation of a colic patient, it is important to note that only about one third of the abdominal contents of a horse can be reached in a rectal exam.
A stomach tube may be passed through the nose to check for reflux or fluid accumulation in the stomach which occurs in some cases of intestinal blockage or impaired motility due to the horse’s inability to vomit.
Further investigation is required in some cases and may include bloodwork, peritoneal taps (removing and assessing some fluid from the horse’s belly using a needle), ultrasound examination orgastroscopy (passing a camera into the stomach). Your veterinarian can determine the need for further work and monitoring, which may require transport to a clinic or hospital facility in some cases.
Some horses appear to be prone to recurrent colic, which is usually seen as multiple bouts of mild to moderate colic which resolve with time or medical treatment.
Investigations including bloods, ultrasound, gastroscopy and other tests can reveal a cause in about 50% of the recurrent cases but usually, even if an underlying diagnosis cannot be made, dietary and management changes can be recommended to reduce the occurrence of these bouts.
Treatment
Usually, treatment can be administered at home and might include sedation, painkillers, antispasmodic drugs, oral or intravenous fluids and management including gentle exercise and withholding feed.
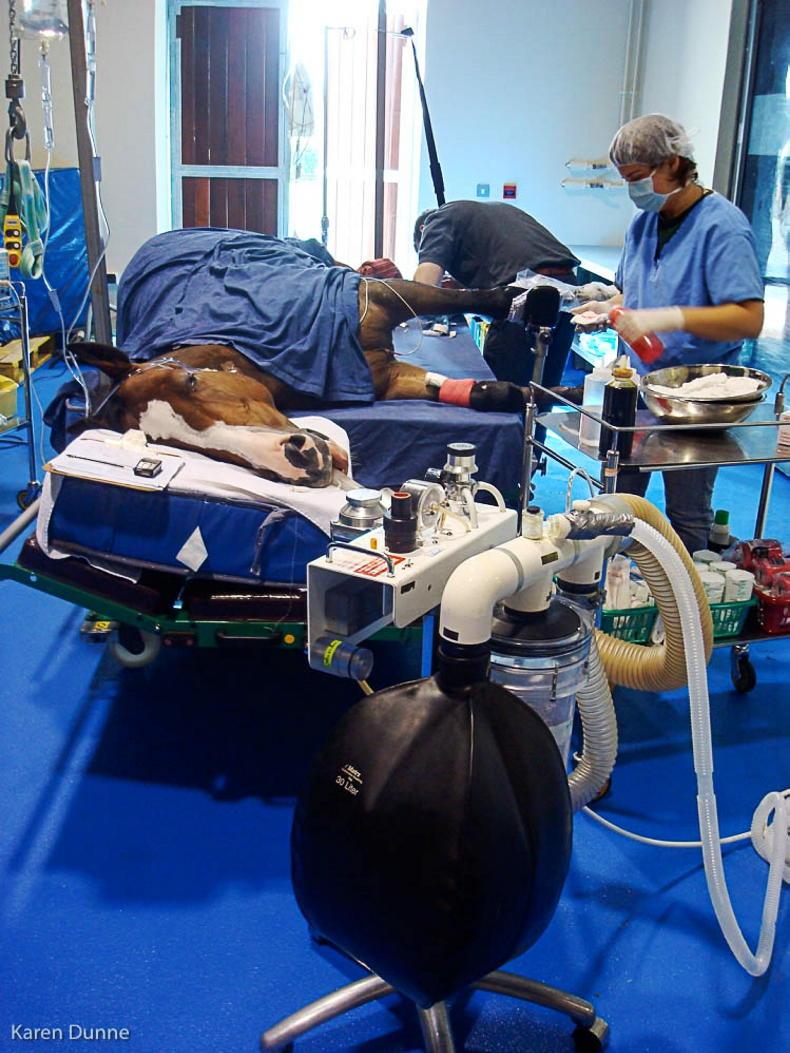
Some cases require repeated treatment, including some impaction colics which can take a day or two to resolve, other cases are better hospitalised for close monitoring and medical treatment such as some cases of displacement colic. In around 10% of colics, surgical treatment is required to save the life of the horse. This may involve re-positioning or untwisting of parts of the bowel and even removal of some sections of the intestinal tract if they have become severely damaged.
The success rates of colic surgery have increased over the last number of years but vary considerably depending on the underlying cause and the amount of damage to the guts.
If surgery is required, the sooner it is performed, the better the chance of a good outcome. Your veterinarian will look for certain clues to indicate whether surgery is required and these can include the heart rate, colour of the gums, presence of reflux, presence of certain changes on rectal exam and a failure to respond to pain relief.
Ultrasound and bloodwork can also be used to confirm if surgery is required but often a definitive diagnosis can only be achieved on the operating table. The decision to undertake surgery is never undertaken lightly given the associated costs and possible complications involved but in many cases rapid intervention can be life-saving.
Unfortunately, no matter what we do, colic can occur in any horse at any time, however good management practices can certainly reduce the risk of it affecting your horse.
Worming: Worms can predispose horses to a number of types of colic by causing irritation of the intestines or affecting how the bowels move. They can also directly cause some types of colic such as ascarid impactions in foals and weanlings where hundreds of noodle-like worms cause a blockage in the gut.
Faecal worm egg counts are a useful tool in a worming programme but not all worms shed detectable eggs so it is important to discuss an appropriate worming programme for your horses with your veterinary surgeon.
Resistance to common wormers is being increasingly reported which means that it is more important than ever to have a good parasite control strategy.
There also seems to have been an increase in the number of cases of larval cyathostomosis, a syndrome of weight loss, colic and diarrhoea associated with immature small redworms which can be fatal. Discuss prevention of this with your veterinary surgeon.
Good feeding practices can help to reduce the risk of colic. Ensure you offer your horse a high-quality diet appropriate for their nutritional needs and make any dietary changes very gradually to avoid upsetting the delicate balance in the horse’s digestive system.
Grazing is the most natural part of the horse’s diet and should be encouraged wherever possible. In stabled horses, fibrous feeds such as hay are far better tolerated by the digestive tract than grains or starchy, sugary hard feeds.
Making sure your horse drinks adequate amounts of water, especially in cold weather or when on box rest, as it will help prevent their gut contents from drying out and forming an impaction.
Adding warm water to drinkers or increasing the water or oil content in feed can be useful. Similarly, ensuring your horse doesn’t gorge himself on straw is important in preventing this type of colic.
Emma Chedgey MVB MRCVS CertAVP(ESM) is veterinary surgeon and director at Lisadell Equine Hospital

THERE are a few useful things you can do to prepare once you have rung your vet to discuss the symptoms. They may give you some instructions over the phone based on the information you provide.
While waiting, it can be worthwhile spending some time gathering information about the horse’s recent diet and management if you have not been responsible for the horse’s everyday care, so you have these answers ready for the veterinary surgeon.
If you don’t know how long the horse has been colicking, try to find out when they were last seen normal or if anything unusual has been noted in the last few days.
Check for clues in the horse’s environment such as droppings (amount and consistency) or signs of rolling/pawing. It can also be useful to have a clean bucket of warm water ready to save time when the vet arrives.
Gently walking the horse may help to distract them and stimulate normal gut movements, however, it is important not to force the horse to walk or wear them out.
Horses that are violently colicking may injure themselves or others so it is a good idea to move them to a safe place such as a sand arena where they are less likely to hurt themselves or get cast.
It is a myth that rolling causes a twisted gut – horses with surgical colics are simply more painful and therefore more likely to persistently roll.
While you are waiting for the vet, remove all feed and try to resist the temptation to administer any medications yourself as these may interfere with the veterinary examinations.
Nothing that you can give at home can ‘fix’ the horse, but it might mask the symptoms and impede accurate diagnosis.
If there is a possibility that surgery will be required, start to think about whether this is an option for your horse, and if so, consider the logistics, such as arranging transport, so you are prepared if your veterinary surgeon advises referral to a hospital.
If your horse is insured, you will probably need to inform the insurance company before surgery is performed so remember to mention this to your vet.


 This is a subscriber-only article
This is a subscriber-only article
 It looks like you're browsing in private mode
It looks like you're browsing in private mode










SHARING OPTIONS: